The makeup of the health care provider workforce in the United States has changed dramatically over the past 20 years. PAs and NPs now deliver 25% of health care in the country. The increasing number of patient encounters involving an Advanced Practice Provider (APP) raises varied opinions and assertions concerning the impact of APPs on health care delivery in the United States.
“It expands access to care.”
“It diminishes the value of physicians.”
“It helps the bottom line.”
“It puts patients at risk.”
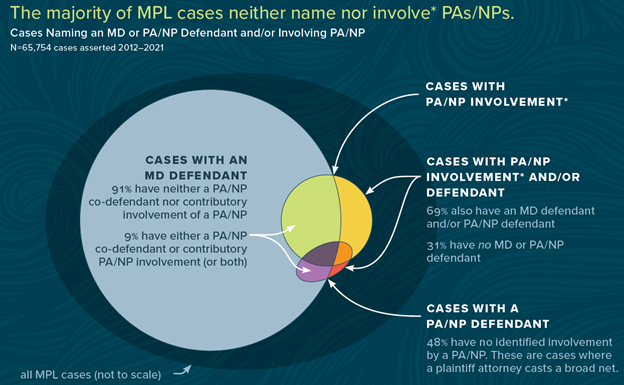
Without starting from any assumptions one way or the other, we set out to identify any insights we could glean through our lens of malpractice data. We examined a total of 65,754 cases asserted between 2012 and 2021. Within this sample, we examined three main groups of cases. There were 45,225 cases in which a physician was named as a defendant. There were 5,506 cases in which the physician assistant or nurse practitioner role was linked to the care, and there were 1,469 cases in which a physician assistant or nurse practitioner was named as a defendant.
Some of the compelling lessons learned were:
- Despite increasing use of advanced practice providers, we do not observe an increase in the proportion of MPL claims involving PAs or NPs
- PAs and NPs are associated with one or more contributing factors in only approximately 8% of all MPL cases, and they are named as defendants in only 2%
- The average indemnity payment is less for cases with only a PA or NP involved compared to cases with just a physician defendant
- Overall, the rate of MPL cases involving physicians steadily dropped from 2012 to 2021. At the same time the proportion of PAs and NPs among health care providers increased by 39%
- Against that backdrop and concurrent with an increase in provider population, PA and NP case trends are flat
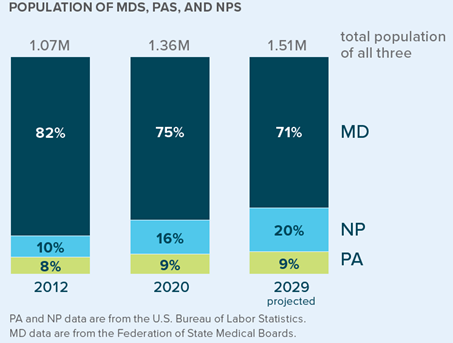
According to the United States Bureau of Labor Statistics, more than 367,000 nurse practitioners and physician assistants were practicing in the U.S. in 2021, a 94% increase from 2012. Over those same 10 years, the number of physicians increased by 19%. By 2029, the increase in the number of MDs is expected to be 3%, while the increase for PAs is expected to be 31% and for NPs the increase is expected to be 52%
The largest proportion of cases involving both NPs and PAs included Diagnosis-related allegations. Surgical treatment was the most common allegation type in MD cases and the second most common allegation for physician assistants. The greatest percentage of cases for NPs, PAs, and MDs occurred in the ambulatory setting.
When looking at the clinical severity, cases involving NPs and PAs had outcomes that were more severe overall than MD cases in general, while cases stemming from high severity injuries (excluding death) were similar for MDs, NPs, and PAs. NP cases had the highest percentage of cases generated by outcomes involving death, however, a multivariate analysis showed that NP or PA involvement alone was not a significant contributor for the outcome of death.
When the care provided by a physician assistant or a nurse practitioner was deemed contributory to a malpractice allegation, the characteristics of such MPL cases were essentially the same whether or not a physician was named as a defendant.
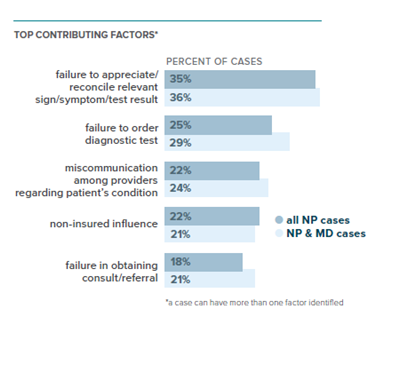
Candello Data Provides Valuable Insights on Top Contributing Factors
(Samples: Candello Database)
Overall, cases involving only PAs or NPs have close-with-payment trends comparable to cases where an MD and a PA/NP were involved. On average, cases involving physician defendants are likely to incur a higher payment whether a PA/NP is also involved or not. Our analysis provides evidence that patient safety and liability risk are generally similar when care involves PAs and NPs compared to MDs.
We undertook this year’s Benchmarking Report to provide data-driven answers to at least some questions surrounding the impact of Advanced Practice Providers on health care delivery and patient safety. This is a subject that affects patients, providers, and organizations alike, and decisions made at every level of the health care system can be influenced by these findings.
The population is aging. This means a growing number of older and more complex patients. At the same time, it also means an aging provider workforce that is moving out of practice, leaving a shortage of qualified providers
Advanced Practice Providers can play a critical role in meeting the needs of patients and health care systems, but there is also a need for information to demonstrate their efficacy and safety
Regardless of the specifics laid out in this report, health care is safest, and MPL risk is lowest, when everyone involved in a patient’s care understands and respects their colleagues and supports their development and growth. Sowing doubt or pointing fingers—whether based on perception or speculation—doesn’t help patients or providers get better. Building on strengths and learning from mistakes, together, enhances everyone’s health care experience.
We hope that this summary of our analysis has been helpful. To review the complete Benchmarking Report, please follow the button below.