When I was a nurse director responsible for managing a medical surgical unit at an academic medical center, my priority was providing opportunities to develop strategies to mitigate risk. The goal was to create safer environments of care for both our staff and patients. The current health care environment is becoming more challenging due to advancing technologies, throughput and capacity concerns and the increasing overall illness acuity of patients—all which are heightening pressures on staff. Leveraging different data can help nurse leaders make data-informed decisions as they work to mitigate risk.
DATA FOR A NURSE LEADER
Patient safety data is a vital tool for health care leaders as it allows us to understand which care processes are most vulnerable so we can evaluate what the opportunities are to mitigate those risks. Greater awareness of why events happen provides the opportunity to focus performance improvements, enhance education and align resources to help prevent future events of patient or staff harm.
A robust safety reporting system provides the insights that are integral to mitigating risk at the operational level. As a nursing director, I would look to our safety reporting data to understand the contributing factors—or steps in the care processes—that caused patient and staff harm. Patient Safety Reports allow the sharing of trended data as well as patient safety stories that can help focus improvement efforts.
When errors were made, we would discuss the events with all the staff involved to better understand what contributed to the events. Was it a work-around to save time; a systems issue; was there confusion or lack of awareness of the policy or procedure? My goal in working with my team was to make sure that if an error was made, we understood why it occurred. This would allow us to develop interventions generated from the staff—those closest to the work—so that we could prevent someone from making the same error in the future.
Transparently sharing safety reporting events and near misses is critical to understand the why, where and how these events happened, and to implement best practices to avoid these events in the future. I reassured staff by telling them, “If this event happened to you, how can we tell this story so that it does not happen to someone else, and more importantly prevents harm to another patient.”
A BROADER LENS
Having a broader picture of the impact of adverse events can sometimes be challenging for nurses and nurse leaders. While we certainly see it at the patient and provider level, we don’t always have line of sight to the overall prevalence of the events, the common contributing factors or the financial impact.
The recent CRICO Strategies Report, The Power to Predict, can offer that wider lens. The report provides trends and analyses in national medical malpractice cases and illuminates the common drivers of patient harm and financial loss patterns related to subsequent malpractice. A nurse leader could access this report to reflect on their own unit’s experience with harm events to see if there are similar vulnerabilities and contributing factors.
REPORT VALIDATES IMPORTANCE OF FOLLOWING POLICIES/PROTOCOLS
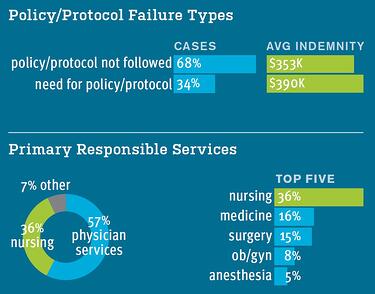 In the report, the analysis of past claims shows that the odds of a malpractice case closing with an indemnity payment increase 145% when the absence of or failure to follow a formal policy or protocol contributed to the patient’s harm. Further, the analysis found that of the cases that involved a failure to have or follow a policy or protocol, nursing was named as the primary responsible service in 36% of the cases.
In the report, the analysis of past claims shows that the odds of a malpractice case closing with an indemnity payment increase 145% when the absence of or failure to follow a formal policy or protocol contributed to the patient’s harm. Further, the analysis found that of the cases that involved a failure to have or follow a policy or protocol, nursing was named as the primary responsible service in 36% of the cases.
As a nurse leader, it was important that I ensured policies and protocols were:
- Meaningful: Did they reflect current practice without being overly burdensome?
- Accessible to staff: Was the staff aware of and adequately trained about the policies?
To ensure that policies are meaningful for the people using them, it is important that those implementing them are at the table when they are in development: identifying potential work-arounds, discussing why certain steps may not be practical, and discussing the best course of action ahead. Their contributions at the development stage help to create clearer and more efficient policies and procedures.
When updating or creating policies, being able to review the national trends in risk and the contributing factors for patient harm—like those offered in this report—offers a broader view of the potential impact of not following a policy.
In addition to physical harms, there are emotional as well as financial impacts. We all recognize that while these failures cause patient harm, they also cause harm to nurses, physicians, care teams, and organizations. My experience with having staff sharing the safety reports with their peers helped to connect the dots for the staff from the error to the overall impact. Adding the data from this benchmarking report for review would enhance that process.
Case Examples from the Report:
A 62-year-old male suffered permanent brain damage due to a fall when he was left alone in the bathroom, contrary to the hospital’s falls risk policy.
A 58-year-old female suffered a broken femur while being transferred to her hospital bed by staff inadequately trained to use a Hoyer lift.
RISK MANAGEMENT STRATEGY
Reading this report offers direction for nurse leaders to evaluate vulnerabilities within their own units.
- Do we have adequate policies to address common risks and are they being followed?
- What is our process for training and monitoring adherence to policies?
- Do we have a process to address cases where there has been a failure to follow established policies?
As a nurse leader it was my responsibility to establish accountability for sharing and educating my staff about the new or revised policies and procedures. Ensuring that all staff had awareness of changes in practice was a crucial part of leadership expectations. Fully appreciating the implications of how new or revised policies influenced the workflow of my staff helped ensure full implementation and the delivery of optimal care.
As nurse leaders, we are better poised to enhance patient safety, if we understand our organization’s culture and risk profile, review national trends, and include relevant staff in the development of solutions.
{{cta('c608b452-f76b-418c-9a8b-f18c108d0518','justifycenter')}}

