Monitoring and Improving Handoffs
Maimonides Medical Center
Problem Statement
Critical patient information miscommunicated during transitions in care
Narrative
It is no secret to health care providers that clinician-to-clinician handoffs are an area vulnerable to miscommunication and, sometimes, tragic results. Fortunately, at Maimonides, we were able to tap into two critical components for discerning the specific underlying causes of inadequate handoffs:
- A way to capture and analyze handoff errors that aligned with the risks commonly present in malpractice cases, and
- A tool (I-PASS) already proven to reduce communication breakdowns during transitions in care.
The data collection and analysis enable us to track how the implementation of I-PASS impacts our specific vulnerabilities, and the tool enables us to standardize a process long left to non-conformity.
Our insurer (Healthcare Risk Advisors/TDC Group) said “We understand that handoffs are risky, we’ll support you to implement I-PASS and measure the impact.”
—Robin Gitman
Vice President for Academic Affairs
The I-PASS tool was developed specifically to improve the handoff process. But complex organizations resist change, and Maimonides is no different. Asking a large cohort of providers to switch to I-PASS from the existing practice needed to be justified with credible data that there was indeed a handoffs problem and reinforced by data tracking the impact of the I-PASS adoption.
To position ourselves as getting ahead of the handoff problem—rather than appearing to belatedly react to the few adverse events that become medical professional liability (MPL) cases—we began working with our residency program. Our theory was, if we help our trainees to see safety problems as an opportunity and then train them to analyze them, then they will learn how to uncover and address specific vulnerabilities throughout their careers.
On a regular basis, we ask our residents to report patient harm events (and near misses) that occurred during a care handoff. Even more specifically, we incorporate the detailed contributing factors coding that the Candello taxonomy applies to handoff-related missteps. This enables us to gauge real and potential harm, the effect of interventions, and the downstream impact on MPL losses. Concurrently—with significant support from our MPL insurer (Healthcare Risk Advisors/TDC Group)—we initiated the use of I-PASS by residents. Once our data collection and analytic capabilities enabled us to use our event reporting system more effectively, the commitment to, and cost of I-PASS training was easily justified.
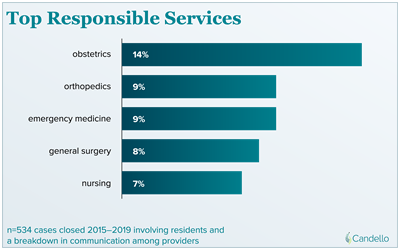
Candello Data Provides Valuable Insights on Miscommunication Involving Residents
(Samples: Candello Database; Not Maimonides-specific)
Data complied by Tarek Zawi, Data Analyst, CRICO
We trained hundreds of residents—and the advanced practice providers they commonly engage during handoffs—then observed the impact. Through direct observation, we can now see how often and how closely residents adhere to the I-PASS format and rate the handoff quality. With that real-time information, we know what needs emphasis or reinforcement in their training and help them become lifelong patient safety leaders.
More from Robin Gitman, VP Academic Affairs, DIO
Centralized Data with CRICO |
Seeing Safety Differently |
CRICO Taxonomy Helps |