Medication-related errors are common, can cause high-severity injuries, and may be costly. Many organizations have made reducing these errors top priority, including the World Health Organization (WHO). In our Candello Report, Medication-related Malpractice Risks, we examine the impact—financial and human—and root causes of medication-related errors.
Every medical malpractice case presents unique circumstances, but a collection of similar cases can reveal a common story of what goes wrong."—Candello Report, Medication-related Malpractice Risks
KEY FINDINGS FROM THE REPORT
This Report examined 3,067 medication-related malpractice cases asserted from 2010–2014. When compared to non-medication events, medication-related malpractice cases involve a larger percentage of deaths and close more frequently with an indemnity payment. Services responsible for most medication errors include general medicine (22%), nursing 13%), orthopedic surgery (5%), and emergency medicine (5%).
Key findings include:
- Primary care providers and hospital-based nurses are particularly at risk
- 32 percent of medication-related malpractice cases involve a patient death, compared with 18 percent of all other cases
- Top medications involved in claims were analgesics (18 percent), anticoagulants (17 percent) and antibiotics (13 percent)
MEDICATION PROCESS
Each step in the medication process—ordering, dispensing, administering, and managing—presents unique risks to providers and their patients, and the 11 percent of cases in which the patient experienced failures in multiple steps demonstrate how intertwined the process can become.
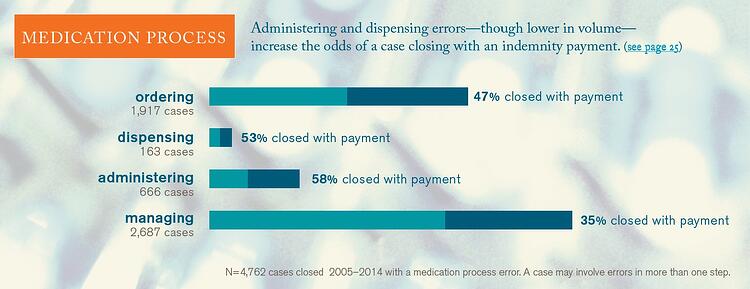
Ordering Errors: From the point a decision is made to order/prescribe a medication until that order is received by the pharmacy or other dispensing service. Examples:
- The clinician ordered the wrong medication for the patient’s condition
- The clinician ordered a medication contraindicated by a patient’s known allergy
Dispensing Errors: From the point the order is received by the dispensing service until it is administered to the patient. Examples:
- The pharmacy dispensed the wrong medication, dosage, or composition
- The pharmacy incorrectly prepared the medication
Administering Errors: The act of delivering the right medication to the right patient in the right dose via the right route at the right time. Examples:
- A prescribed medication was administered to the wrong patient
- A prescribed medication was not administered on schedule, or at all
Monitoring and Management Errors: From the point the patient receives a medication, including renewals, until he or she is no longer taking it. Examples:
- A patient’s adherence to his/her medication regimen was inadequately monitored/assessed
- A patient’s physiological response to new, changed, or short-term medications was inadequately monitored/assessed
Analyzing medical malpractice data enables organizations to identify opportunities along the medication process for improvement to reduce medication-related patient safety risks. To understand the contributing factors involved in each step of the medication process, download the full report.
“There has been a greater willingness to see improving the medication process as a multidisciplinary effort. Errors are not a “prescriber” problem, nor a “pharmacy” problem, nor a “nursing” problem: everybody owns the problem because there are opportunities for errors and harm in medication management.” Frank Federico, RPH | Institute for Healthcare Improvement
WHAT WORKS: MITIGATING MEDICATION-RELATED RISKS
Several efforts to reduce medication-related adverse events have been implemented across a variety of health care systems or developed by organizations like the Centers for Disease Control (CDC) which are highlighted in the Candello Report. They include:
- Pain Medication Management: Professional liability insurers, MMIC and UMIA, part of Constellation, identified medication-related vulnerabilities among nearly 20 percent of their medical malpractice claims and worked with their insureds to develop risk mitigation programs.
- Re-engage Patients in Anticoagulation Treatment Plans: Beth Israel Deaconess Medical Center (BIDMC) implemented a program to re-engage patients who are not following their treatment plans.
- CDC Antibiotics Stewardship Programs: The CDC has a program that focuses on antimicrobial therapy and ways to reduce unnecessary use of antibiotics through antibiotic stewardship.
- Educating providers and patients: Institute for Safe Medication Practices (ISMP), now affiliated with ECRI, works to prevent medication error through medication safety publications for health care professionals and consumers.
- Putting a stop to inadvertent medication discontinuation: Main Line Health System identified an opportunity for improvement associated with automated stop orders on routine medications.
National leaders in patient safety who contributed to the Report include, Frank Federico, RPH, Vice President, Institute for Healthcare Improvement, Michael Cohen, RPh, President, Institute for Safe Medication Practices, David Bates, MD, Senior Vice President & Chief Innovation Officer, Brigham & Women’s Hospital, and Argin Srinivasan, MD, FSHEA, Associate Director for Healthcare Associated Infection Prevention Programs, Centers for Disease Control and Prevention.
